Specialty drugs account for more than half of total drug spend and are often the largest cost driver for employer pharmacy plans. A recent BenefitPRO article points to biosimilars as a practical solution — and for MedBen Rx clients, the effect is already clear, with employers reducing their average monthly spend on these medications by 78%.
Despite MedBen Rx clients experiencing proven success, biosimilar adoption still lags with many other PBMs, due to rebate structures tied to high-priced medications that distort the true cost of care, making expensive therapies seem competitive while more affordable options like biosimilars are overlooked.
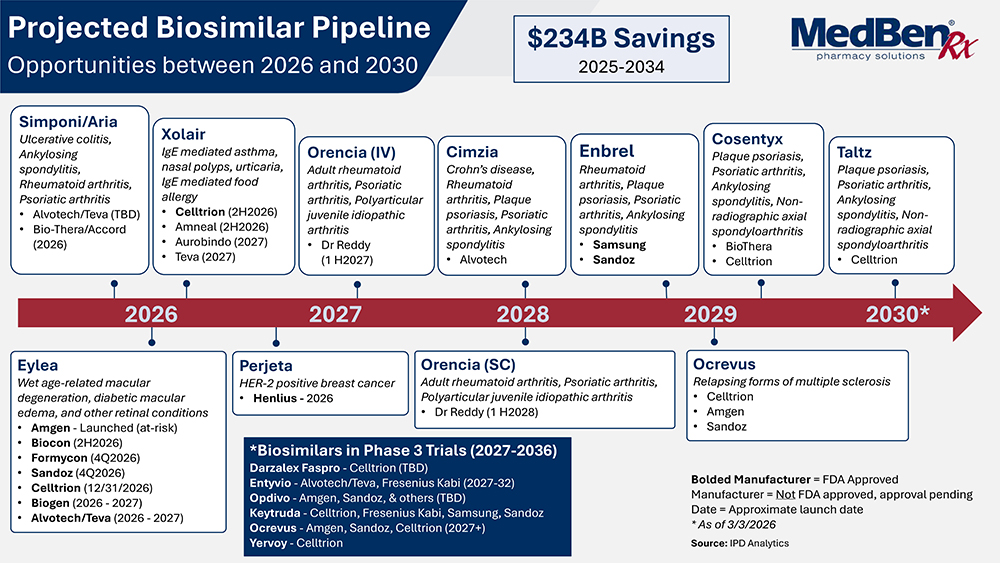
However, momentum is building. With nearly 120 biologics expected to lose patent protection over the next decade, the biosimilar pipeline is expanding rapidly. Employers can secure immediate savings while positioning plans for further price declines through higher competition.
Capturing this value requires strategic pharmacy plan design: prioritizing transparency, moving away from rebate-centric models, and making lower-cost biosimilars a default option.
